Anthrax Fact Sheet
 |
Anthrax (Bacillus anthracis, Malignant pustule, Malignant edema, Woolsorter disease, Ragpicker disease) ICD-9 022; ICD-10 A22 |
Agent: Bacillus anthracis, a gram-positive rod, may be an effective biological weapon because it is easy to cultivate, readily forms spores, and can be aerosolized. B. anthracis spores remain viable for years, infecting soil and other materials long after initial attack.
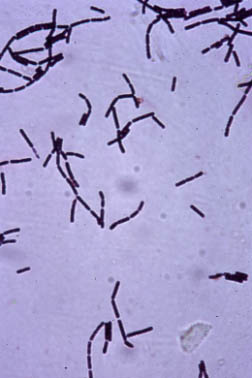 Anthrax Gram Stain Zoom In  |
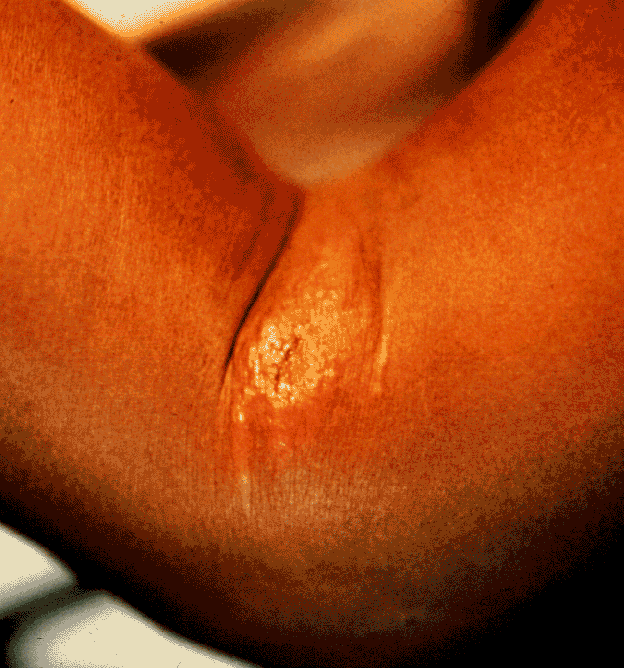
Cutaneous Lesion, Day 1 |
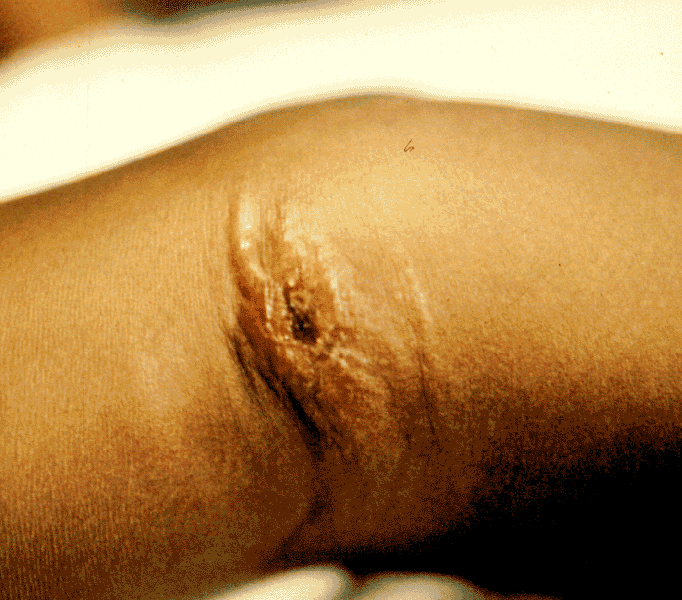
Cutaneous Lesion, Day 2 |
Reporting Requirements for Disease: Immediately report any suspect cases of respiratory, cutaneous, or gastrointestinal anthrax to your local health authority; or, call the Texas Department of State Health Services at 1-800-252-8239.
Infection Control: Standard Precautions should be practiced. Gloves should be worn for contact with cutaneous lesions. Surfaces should be washed with a sporicidal agent such as 0.5% sodium hypochlorite (1 part household bleach added to 9 parts water). Persons exposed to the aerosol should shower thoroughly with soap and water.
Incubation Period: 1-60 days for respiratory and 1-12 days for cutaneous.
Signs/Symptoms: Patients with respiratory anthrax usually have a biphasic illness. Initially, nonspecific symptoms such as malaise, fever, chills, myalgias, and fatigue may appear; upper respiratory symptoms such as coryza, nasal congestion, and sneezing are usually absent. Cough (usually nonproductive) may be present early or late. The patient may show signs of improvement after 2-4 days. These symptoms are then followed by a sudden onset of severe respiratory distress with dyspnea, diaphoresis, stridor, and cyanosis. Chest wall edema may be observed. Hematogenous spread may result in such nonrespiratory symptoms as headache and abdominal pain, nausea, and vomiting. Physical findings are nonspecific except that rhonchi may be present. Without treatment, shock and death follow within 24-36 hours of onset of severe symptoms.
With cutaneous anthrax, patients typically present 1-7 days after exposure with a papule that progresses to a 1- to 2-cm vesicle with serosanguinous fluid; satellite vesicles may be present. This lesion coalesces into an ulcer with a characteristic coal-black scab (eschar; hence anthrax from the Greek for coal) that separates and falls off in 2 to 3 weeks regardless of treatment. The lesion may be intensely pruritic, and although the lesion itself is not painful the associated edema may be painful. Patients may have systemic symptoms such as fever/chills and headache. Left untreated 20% will prove fatal.
Diagnosis:
Differential Diagnosis: The prodromal phase of respiratory anthrax resembles influenza; however coryza, nasal congestion, and sneezing are typically absent with anthrax and influenza has a more rapid progression (usually far less than a day). Many other systemic infectious diseases may mimic the prodrome of respiratory anthrax. Other potential bioterrorism agents that may be associated with flu-like prodromes (Yersinia pestis, Coxiella burnetii, Francisella tularensis, and smallpox) need to be considered for an unexplained cluster of patients (ie, wrong season, wrong age, negative tests for influenza). Plague, Q fever, and tularemia can also cause severe respiratory symptoms and pneumonia. An aerosol exposure to staphylococcal enterotoxin B (SEB) can cause the abrupt onset of severe respiratory symptoms. As usual, common causes of pneumonia must be excluded in febrile patients who progress to respiratory distress. The lesions of cutaneous anthrax must be differentiated from those associated with brown recluse spider bites, which may or may not be painful and produce an eschar, as well as the usually painful lesions associated with staphylococcal or streptococcal skin infections, ulceroglandular tularemia, plague, herpetic involvement of an extremity, and orf. Although cat scratch disease usually causes significant lymphadenitis, a pustular lesion may or may not be recalled.
Diagnostic Tests: A widened mediastinum on chest x-ray or CT is highly suggestive of pulmonary anthrax; pleural fluid may also be evident. In pulmonary anthrax, Bacillus anthracis bacilli (not spores) or genetic material may be detectable 2-3 days postexposure (and sometimes later) by Gram stain, routine culture, or PCR of blood, buffy coat, or pleural fluid. PCR or ELISA may sometimes detect protective antigen in serum. Organisms are not typically seen in the sputum since pneumonia is rare. Hemorrhagic meningitis is common and organisms may be identified in CSF. In cutaneous anthrax the organisms can be detected by Gram stain and culture of aspirates from the lesion, but are rarely in blood. Rectal swabs are only used if gastrointestinal anthrax is suspected. The bacilli are not highly infectious, and the spores, which are, are not found within the body unless it is open to ambient air.
Specimen Submission: All specimens must be triple contained in an approved shipping container and have biohazard labels. Before transport is arranged, the receiving laboratory must be alerted prior to transport by calling (800) 252-8239 ("press 1"). Newly available diagnostic tests may be discussed at that time. There is no specific hazard to personnel handling specimens unless they contain spores. Specimens must be accompanied by a Specimen Submission Form and submitted to the Texas Department of State Health Services Laboratory, 1100 West 49th Street, Austin, TX 78756. Instructions for filling out the G-2A submission form for curtures and the instructions for filling out the G-2B submission form for serology.
Additional Tests: Neutrophilic leukocytosis is often revealed upon laboratory evaluation. Pleural and cerebrospinal fluids may be hemorrhagic. Pleural effusions with or without infiltrates may be evident on chest x-ray.
Treatment: Cutaneous anthrax in adults (including pregnant women) should be treated with ciprofloxacin 500 mg po bid or doxycycline 100 mg po bid for 60 days. Children should be treated with ciprofloxacin 10-15 mg/kg po every twelve hours (not to exceed 1g/day) or doxycycline. Doxycycline dosage is as follows:
> 8 yrs and > 45 kg: 100 mg po every 12 hours
> 8 yrs and ≤ 45 kg: 2.2 mg/kg po every 12 hours
≤ 8 yrs: 2.2 mg/kg po every 12 hours
Patients who have extensive edema, lesions on the head or neck or systemic involvement should be treated with IV combination therapy (see treatment for inhalational anthrax). Inhalational anthrax is often fatal if treatment is begun in the second stage of the illness. Historically, penicillin has been the treatment of choice. However, naturally resistant strains occur, and it is relatively easy to induce penicillin and tetracycline resistance in the laboratory. In the absence of sensitivity data, treatment should be instituted with ciprofloxacin 400 mg IV q12h or doxycycline 100 mg IV q12h. Children should be treated with ciprofloxacin 10-15 mg/kg IV q 12 hours (not to exceed 1 gm per day) or doxycycline at the same dosages as for cutaneous anthrax; however, the doses are given by the intravenous route. If the organism can be shown to be penicillin sensitive, therapy can be instituted with penicillin G 2 million units IV q2h for adults. Children could also be treated with penicillin at high pediatric doses. Clindamycin should be added to whichever regimen is chosen for therapy. Therapy should be continued for 60 days. Patients with meningitis should be treated with high dose penicillin as above or chloramphenicol 15 mg/kg IV q 6 hours. Rifampin may be added to this regimen. Pregnant women may be treated with all of the above medications except rifampin. If the organism is susceptible to penicillin, therapy for pregnant women may be switched from ciprofloxacin or doxycycline to penicillin. Supportive therapy including appropriate vasopressors and oxygen may be necessary.
Vaccines: Anthrax Vaccine Adsorbed (AVA- Bioport Corporation) is the only licensed vaccine in the United States. The vaccine is administered as a 0.5ml subcutaneous injection at 0, 2, and 4 weeks with booster doses at 6, 12 and 18 months. Annual boosters are recommended if immunity is to be maintained. Adverse events included local reactions of edema/induration alone (1%), systemic reactions of fever, chills, and body ache (<0.06%). Precautions for administration include pregnancy. Contraindications include a) anaphylaxis to previous doses of anthrax vaccine or subcomponents of the vaccine (benzethonium chloride, aluminum hydroxide) and b) individuals with prior proven anthrax infection should not receive the vaccine as they are more likely to experience severe vaccine reactions.
Prophylaxis: Ciprofloxacin 500 mg bid po or doxycycline 100 mg bid po should be given for 4 weeks if the patient is vaccinated. Those with fewer than three doses of vaccine should receive a single 0.5 ml booster. If unvaccinated, patients should receive vaccine according to the schedule above. If vaccine is unavailable, antibiotic therapy should be continued for 60 days. If penicillin sensitivity is established, prophylactic therapy can be switched to amoxicillin 500 mg q8h po. Prophylaxis can be administered to children with ciprofloxacin 10-15 mg/kg po q 12 h (not to exceed 1 g per day) for 60 days, doxycycline:
8 yrs and > 45 kg: 100 mg po every 12 hours
8 yrs and ≤ 45 kg: 2.2 mg/kg po every 12 hours
8 yrs: 2.2 mg/kg po every 12 hours for 60 days
Or, if penicillin sensitivity is established,
Amoxicillin:
Weight ≥ 20 kg: amoxicillin 500 mg po q 8 h
Weight < 20 kg: amoxicillin, 40 mg/kg divided into 3 doses taken q 8 h for 60 days.